About Caregiving
by the NCPC
Introduction
Characteristics Of Those Receiving Care
Characteristics Of Caregivers
The Cost Of Caregiving
Trends In Caregiving
The Plight Of Informal Caregivers
Conclusion
INTRODUCTION
Caregivers provide assistance to other people who because of physical disability, chronic illness or cognitive impairment are unable to perform certain activities on their own. So-called informal care can be offered by family members or friends, often in a home setting. Or paid or volunteer professional care, so-called formal care, can be obtained at home, in the community or from institutions such as nursing facilities or government institutions.
Roughly, 11.1 million Americans of all ages are receiving formal or informal care at any given time. This represents about 4% of the population and is comprised of about 9.5 million receiving care at home or in the community and another 1.6 million residing in nursing or intermediate care facilities. About 25.8 million family caregivers provide personal assistance to individuals 18 years or older who have a disability or chronic illness. And nearly one out of every four households (22.4 million households) is involved in giving care to persons aged 50 or older. About 43% of those receiving care are under the age of 65 and are evenly spread between ages 18 to 64. Children under 18 and receiving assistance because of disability are often characterized under different criteria of caregiving.
Sometimes human caregivers can be replaced or assisted by mechanical devices. These might include special computer systems for communication, special locomotion equipment, remote vital sign monitoring devices or remote oversight monitoring. Continued technology advances may help relieve the time commitment of human caregivers.
Since the implementation of the Medicare Prospective Payment System in 1999, home health agencies have been looking for more cost-effective ways to provide care. Telehomecare is a more effective way to deliver home care under certain circumstances. Since it is a rapidly developing field, it's difficult to define all telehomecare applications.
It usually involves two-way electronic communication between the patient and the formal caregiver such as a nurse or doctor. Communication can occur with two-way radio, telephone or as is usually the case, two-way interactive video using a computer and phone lines or satellite downlink. This electronic face-to-face home visit also requires some means for the care provider--who might be hundreds of miles away-- to access patient vital signs and receive patient-initiated medical tests. The patient or her in-home informal caregiver has been trained to use electronic monitoring or test equipment that sends the relevant video snapshots or numeric data via phone line, or radio wave to the formal caregiver.
Telehomecare is not only more cost-effective but also in many cases it provides a higher quality of care. Here are some of the ways telehomecare is proving to be beneficial:
- reducing number of visits to the emergency rooms
- reducing unnecessary visits to physician's offices
- avoiding unnecessary costly visits by health providers
- providing education of the patient in early symptom management
- monitoring vital signs on a 24-hour basis, therefore providing a potential for early intervention and/or prevention of repeat hospitalization
Although electronic monitoring of patients is also a function of telehomecare, it is also becoming a primary source of supplemental home care service not always involving the use of a home health agency. This area of assistance focuses more on the use of devices that warn of problems with homebound people who are often without caregivers for certain periods of the day. This may include 24-hour vital sign monitoring, video surveillance, emergency signaling systems or GPS locator devices for wandering care recipients.
CHARACTERISTICS OF THOSE RECEIVING CARE
Those people requiring the assistance of a caregiver generally fall into 3 categories: Acute care patients, chronic care recipients and younger individuals with permanent mental impairment requiring supervision.
Acute Care
Acute care is often a rehabilitative recovery from a hospital stay or it may be a recovery from a serious illness or injury. With acute care, the individual is typically under the formal supervision of a nurse, physical therapist or nurse's aide. Recovery can be at home but is more likely to be in a hospital rehab wing or skilled nursing facility. Recovery time is usually a matter of a few weeks or months after which the person–even if not completely whole-- is typically capable of not needing a caregiver to function normally.
Acute conditions that may require the assistance of a caregiver might be recoverable brain damage or spinal cord injuries and orthopedic traumas or elective orthopedic surgery, especially to the back or feet, which are slow to heal. Other serious injuries from accidents may also require formal or informal caregiving. Serious acute circulatory conditions such as a heart attack, mild stroke or infectious diseases of the heart or blood vessels may require a caregiver. Cancers, especially the types affecting the abdominal cavity, may require a caregiver before death or recovery occurs. And many severe infectious diseases may result in a recovery period where the patient is too weak and needs a caregiver.
Chronic Care
Certain diseases, disorders, accidents or injuries result in disabilities that last longer than a few weeks or months. Many of these become permanent problems and although the disabled person may eventually adapt to take care of himself, a caregiver is often needed. The location of where this care is given, either in the community or in an institution and whether the care is provided by informal or formal caregivers is dependent on the nature of the disability and the ability of the caregiver.
Constraints on the ability of an informal caregiver to watch over a loved one are:
- the amount of time needed to care for the disabled
- the need to balance a job with the demands of caregiving
- the need for medical supervision of the disabled person
- the physical demands of moving the disabled
- the issue of the dignity and privacy of the caregiver and the disabled over changing dirty diapers or helping in the bathroom with toileting and bathing.
Often an informal caregiver will attempt to provide this care perhaps out of love or a sense of obligation, but a better solution for everyone involved might be the use of a formal caregiver such as a home health agency or an assisted living facility. The nature of the chronic condition also dictates who gives care and where.
Many informal caregivers attempt to cope with care beyond their ability or expertise. Added to this pressure is the fact that the care recipient is often reluctant to give up the familiar environment of the home in favor of what might be better care and a more stimulating environment in an assisted living facility or a nursing home.
Chronic conditions resulting in permanent care might include permanent spinal cord or brain damage, disabling strokes, advanced congestive heart failure, various dementias such as Alzheimer's Disease, Parkinson's Disease, emphysema, various hereditary disorders such as Huntington's Disease, advanced diabetes, obesity-induced joint failure, disabling amputation, chronic disabling pain caused by injury or diseases such as pancreatitis, advanced osteoarthritis especially of the back, advanced osteoporosis with stress factors, AIDS and a host of slow-acting incurable cancers.
Many of the above problems are more prevalent with advanced ages and as a rule, caregiving is a problem associated with aging. But many people of all ages often develop disabling conditions requiring care. And many of these are progressive forms of auto-immune disorders such as type I diabetes, rheumatoid arthritis, multiple sclerosis, scleroderma, lupus, ALS, muscular dystrophy, myesthenia gravis, and many more.
Mental impairment developed early in life
Many of the roughly 5 million persons between the ages 18 to 65, requiring caregivers, are impaired due to mental retardation, autism, Down's Syndrome, mental illness or severe depression. Many will live an entire lifetime needing supervision and because they have such a long-term need their numbers tend to skew the data for age-related caregiving. Although no studies are available showing the incidence of first-time caregiving-–number of people per 10,000 needing care each year for the first time–-this incident rate would probably be very low for young-aged individuals and high for the old-aged.
For people over age 65, the average need for care is probably only 2 to 4 years before recovery or death. With the aged there is a constant turnover of new cases replacing those who die or recover. With the mentally impaired, the need for care may drag on for scores of years. There is less turnover due to death or recovery and these unfortunate people tend to accumulate in number.
Although many of these people are cared for at home under supervision of their family, many more are cared for in special facilities licensed for this type of care. Both formal and informal caregivers are supported by government programs to help relieve the financial burden this type of caregiving can impose.
CHARACTERISTICS OF CAREGIVERS
Custodial Care versus Skilled Care
Custodial care and skilled care are terms used by the medical community and health care plans such as health insurance plans, Medicare, Medicaid and the Veterans Administration. They are used primarily to differentiate care provided by medical specialists as opposed to care provided by aides, volunteers, family or friends. The use of these terms and their application is important in determining whether a health care plan will pay for services or not. Generally, skilled services are paid for by a health care plan and custodial services, not in conjunction with skilled care, are not covered. However, custodial services are almost always a part of a skilled service plan of care and by being included, custodial services are paid by the health care plan as well. Many people have the misconception that only skilled services are covered. This is simply not true.
According to the American College of Medical Quality:
" Skilled care is the provision of services and supplies that can be given only by or under the supervision of skilled or licensed medical personnel. Skilled care is medically necessary when provided to improve the quality of health care of patients or to maintain or slow the decompensation of a patient's condition, including palliative treatment. Skilled care is prescribed for settings that have the capability to deliver such services safely and effectively.
Custodial care is the provision of services and supplies that can be given safely and reasonably by individuals who are neither skilled nor licensed medical personnel. The medical necessity and desired results of skilled care must be clearly documented by a written treatment plan approved by a physician. A patient may have skilled and custodial needs at the same time. In these circumstances, only those services and supplies provided in connection with the skilled care are to be considered as such. The treatment plan must include:
• The applied therapies;
• The frequency of the treatment which is consistent with the therapeutic goals;
• The potential for a patient's restoration within a predictable period of time, if applicable;
• The time frame in which the prescribing physician will review the case for the purpose of evaluating a patient's status and before reassessing the medical necessity of ongoing treatment; or
• The maintenance, palliative relief, or the slowing of decompensation in a patient's status, if applicable.Determinations of the medical necessity of skilled care must be based on the applicable standard of care."
Writers and advisers who are not part of the medical community often confuse custodial care and skilled care with specific care activities. For example help with the activities of daily living and many of the items on the list in the previous section are care activities thought to be by definition custodial care. Whereas the monitoring of vital signs, ordering medical tests, diagnosing medical problems, administering of intravenous injections, prescribing and dispensing medicine, drawing blood, giving shots, dressing wounds, providing therapy and counseling are all activities normally associated with skilled care.But many non-medical advisers and writers don't know that skilled and custodial refer to the people who deliver the care not the actual care given.
A skilled care provider can also provide services normally thought to be provided by custodial caregivers. Such things as help with activities of daily living and so-called instrumental activities of daily living are often furnished by skilled providers in the course of their treatment. Or a skilled care plan may call for services that can be delivered by a custodial caregiver but it would still be under the skilled plan of care for that individual. On the other hand people who deliver custodial services may from time to time perform those activities supposedly reserved for skilled providers. Such things as taking blood pressure, administering medicines, giving shots or changing wounds might be provided under certain circumstances by a custodial provider.
Please remember that the terms skilled and custodial do not refer to specific types of long-term care services but rather who delivers those services. Also the delivery of skilled services must be done under a written plan of care which often includes custodial care services.
Does Medicare Cover Custodial Care?
Of course it does. Medicare routinely pays for custodial care in every skilled care setting for which it provides payment. Medicare will not pay for custodial care in the absence of a skilled care plan.
Medicare covered nursing home stay
A patient receiving skilled care in a nursing home from Medicare not only receives care from skilled providers such as nurses, therapists or doctors but also receives care from custodial providers such as aides or CNA's. This care usually consists of help with bathing, dressing, ambulating , toileting, incontinence, feeding and medicating. Medicare does not exclude the custodial services but pays the entire bill because custodial care is a necessary part of the skilled care plan in a nursing home.
Medicare covered home care
Custodial care is always a part of a skilled care plan for home care. The patient receives skilled care from a nurse or therapist and custodial care from an aide for help with bathing, dressing, ambulating , toileting, incontinence, medicating and possibly feeding. Medicare pays for both types of services.
Medicare hospice care
The hospice team consists of a doctor, a nurse, a social worker, a therapist when needed, a counselor and an aide to provide custodial care. Help with activities of daily living is provided at home or in a Medicare approved hospice facility. Custodial care is always a part of a hospice plan of care and Medicare routinely pays for these services.
Please note that there is no such thing as a custodial nursing home. All nursing homes are by definition skilled care facilities because they have nurses who are skilled care providers. Also be aware that not all states license intermediate care facilities which might provide less than 24 hour registered nursing care. "Skilled care patients" in nursing homes are referred to as such because they are receiving payment from Medicare or sometimes payment from private health insurance plans. Practically all nursing home residents have medical needs but Medicare and other insurance plans will only pay for patients that have certain acute medical needs where recovery is anticipated. Patients with chronic medical problems are typically not covered by Medicare but would be covered by Medicaid.
The confusion with understanding the term "skilled nursing care" probably comes from Medicare itself. To be a certified Medicare nursing home and receive payments from Medicare a nursing home must meet the Medicare definition of a "skilled nursing facility". This means there must be registered nurses on duty 24 hours a day, there must be a doctor on call at all times and there must be ambulance service to a local hospital. Medicare may also require additional staffing and facility arrangements to receive certification. It is unfortunate that the word "skilled" is used in this definition. All nursing homes whether they meet the definition of a "skilled nursing facility" or not provide services from a nurse, doctor or therapist and this meets the medical definition of skilled care. Many states have adopted the same federal criteria for licensing their nursing homes. In some states the "skilled" definition is the only option for a nursing home. But in some states facilities with lesser services can receive different licensing classes. These might be called intermediate care facilities or "small nursing homes".
Formal Caregivers
Formal caregivers are volunteers or paid care providers associated with a service system. Service systems might include for-profit or nonprofit nursing homes, intermediate care facilities, assisted living, home care agencies, community services, hospice, church or charity service groups, adult day care, senior centers, association services, state aging services and so on. More detail on the services, availability and costs of nursing homes, assisted living facilities and home care agencies are provided in other sections of this site.
During 1998, in the U.S., 9.5 million patients were served by home health agencies and 576,000 by hospice care. This care was provided by approximately 13,000 agencies, nationwide. The percent distribution of disorders requiring home care were: diseases of circulatory system–25.2%, injuries and poisoning–9.9%, muscle and skeletal disease–8.8%, respiratory–8.4%, cancer–7.3%, endocrine, nutrition, metabolic, immune–5.4%, nervous system– 4.3%, others–balance of distribution. Of the patients served by hospice, about 76% had cancer or heart disease.
In 1997, there were about 17,000 skilled and intermediate term nursing homes in the US serving 1,609,000 residents. About 1,465,000, or 91% of residents, were age 65 and older. Out of those 1.5 million elderly patients in nursing homes in 1997, as a percent of the total, help was provided with 1 or more activities in the following categories: bathing or showering–96.2%, dressing–87.2%, using toilet room–56.2%, eating--45%, transferring to chair or bed–25.4%.
As of the year 2000, an estimate by NatWest Securities places the total number of assisted living beds nationwide at 1,387,836 beds with total revenue of $33.1 billion. Although assisted living facilities (ALFs) are regulated by the state health departments, data for utilization and cost don't show up in national statistics. And although Medicaid covers some cost for ALFs, the costs of numerous waiver systems used by states aren't shredded out separately.
The numbers of people using ALFs are included in those 9.5 million receiving care in the community. A 1996 survey by the American Health Care Association reveals that 59% of ALF residents are admitted from their homes and the other 41% come from nursing homes, hospitals or other ALFs.
Some ALFs have found a niche in providing care to Alzheimer's patients and many ALFs are exclusively dedicated only to Alzheimer's residents. This disorder requires constant supervision but not necessarily from the more costly skilled medical staff found in nursing homes. And since at least 5% of those over 65 and 46% of those over 85 suffer from mental impairment, this provides a potentially large market for ALF Alzheimer's facilities
Not all residents of ALFs need care or assistance. Many are there because they want a simpler lifestyle without the worry of maintaining a home and they seek the companionship of other people their own age. They have chosen assisted living because they may need some minor help with IADLs but they anticipate a time when they may need the more intensive care available with an ALF.
As of 1996, ALF residents who were independent with ADLs (needing no assistance) were as follows: eating--88%, transferring--84%, toiletting--78%, dressing--58%, bathing--49%. A recent survey of assisted living administrators estimated that 24% of their residents received assistance with 3 or more activities of daily living, such as bathing dressing and mobility. They estimated that about one-third of residents had moderate to severe cognitive impairment.
Informal Caregivers
Informal caregivers are family, friends, neighbors or church members who provide unpaid care out of love, respect, obligation or friendship to a disabled person. These people far outnumber formal caregivers and without them, this country would have a difficult time formally funding the caregiving needs of a growing number of disabled recipients.
Depending on the definition of caregiving, estimates of the number of informal caregivers range from 20 million to 50 million people. This could represent about 20% of the total population providing part-time or full-time care. The typical caregiver is a daughter, age 46, with a full-time job, providing an average of 18 hours per week to one or more of her parents.
Among adults aged 20 to 75, providing informal care to a family or friend of any age, 38% care for aging parents and 11% care for their spouse. About two-thirds of those caregivers for people over age 50 are employed full-time or part-time and two-thirds of those–about 45% of working caregivers–report having to rearrange their work schedule, decrease their hours or take an unpaid leave in order to meet their caregiving responsibilities.
A recent study estimates these people lose about $660,000 in wage wealth over their lifetime because of work sacrifices. And estimates of productivity losses to businesses because of time off for caregiving range from $11 billion to $29 billion yearly. The average amount of time informal caregivers provide assistance is 4.5 years but 20% will provide care for 5 years or longer.
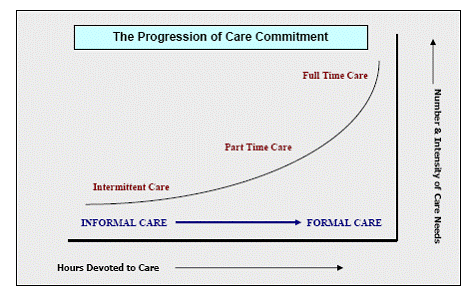
Understanding the Progression of Care Commitment
The chart below illustrates the relationship of informal care to formal care. As care needs increase, both in the number of hours required and in the number or intensity of activities requiring help, there is a greater need for the services of formal caregivers. Unfortunately, many informal caregivers become so focused on their task they don't realize they are getting in over their heads and they have reached the point where some or complete formal caregiving is necessary. Or the informal caregiver may recognize the need for paid, professional help but does not have the money to pay for it.
It is the job of a care manager or a financial adviser or an attorney to recognize this need with the client caregiver and provide the necessary counsel to protect the caregiver from overload. An overloaded caregiver is likely to develop depression and/or physical ailments and could end up needing long-term care as well. Or the consequences of not being able to cope with caregiving might even result in an early death for the caregiver.
Intermittent Care
This would require the occasional attention of an informal caregiver but there may also be a medical condition that may require expertise the informal caregiver does not possess. As a general rule most people receiving this kind of care would probably be in their own home and the caregiver would be living or working close by and stop only for occasional visits.
There is, however, a growing trend where the only family caregivers may be living hundreds or thousands of miles away from their loved one. In this case, a care manager would be hired to arrange for the intermittent care for the loved one.
Part Time Care
This could still be furnished by an informal caregiver assuming there is no extensive medical condition requiring frequent attention. It is more likely under this scenario the care-recipient and the informal caregiver would be living together. Or with no caregiver available a decision would have to be made whether it would be in the best interest of the care-recipient to receive formal care in the home or to go to a care facility. Oftentimes a care facility can offer a better environment at a lesser cost. On the other hand, many care-recipients prefer to remain in their homes at all costs. And for long distance caregivers, hiring a care manager is still the best option.
Full-Time Care
Full-time care can often be offered by informal caregivers living with the care-recipient. But this arrangement is not always in the interest of the caregiver. Because of the demand on a caregiver's time and attention, this arrangement will often result in the caregiver suffering from severe depression, social isolation and the development of medical ailments. Again, the decision is often dictated by the lack of funds to pay for professional care. But when the need for care has progressed to a fulltime basis, advisers or family should be looking to implement formal care delivery either in the home or in a facility. As with the other care options above, a care manager could prove invaluable in selecting the setting and the care providers.
Depending on what causes the need for long-term care, a care-recipient could start out at any point on the curve below. For instance a stroke, injury or sudden illness may result in the immediate need for part time or fulltime care. On the other hand the slowly progressing infirmity of old age, the slow onset of dementia or a progressively deteriorating medical condition may only require occasional help; beginning with intermittent care from an informal caregiver but gradually progressing to the need for fulltime, formal care.
THE COST OF CAREGIVING
One of the biggest concerns of elderly Americans is the high cost of medical care. There are 35 million people over the age of 65 in this country and they comprise 12.8% of the population.
Despite the fact that the elderly comprise only 12.8% of the population, they consumed at least 24% of all health expenditures in 1997 in the form of Medicare and Medicaid outlays. This demonstrates that health care for the elderly is costing more per year on average than for younger age groups.
A 1996 survey by Medicare reveals average yearly total health care costs (service, insurance premiums and drugs) as follows: ages 65 to 69--$5,864, ages 70 to 74--$6,744, ages 75 to 79--$9,414, ages 80 to 84--$11,256, ages 85 and older--$16,465. For these older ages, the primary reason for the 3 fold increase in cost from age 65 to age 85 is the cost of caregiving.
It is estimated that only about 9% of 65 to 69 year-olds are receiving help from a caregiver whereas about 50% of the age 85+ are receiving care. About half of all nursing home residents are 85+. And use of home care for the very old is also higher. Between 1998 and 1999, home health agencies made 2,350 visits for every 1,000 enrollees aged 65 to 74, compared with 12,709 per 1,000 for enrollees aged 85+.
It is the high cost of long-term care that should worry older Americans more than the cost of medical services, drugs or health insurance premiums. In 1996 older Americans living in nursing homes incurred $38,906 in annual health care expenditures on average, compared with $6,360 among older persons living in the community. Nursing home accounted for 64 percent of total expenditures of the institutional population.
The need for receiving long-term care increases as a person ages. And the probability of needing care becomes very high for the very old. It should also alarm elderly Americans that the ranks of the very old are growing at astronomical rates. Those over age 85 are the fastest growing population group in the nation.
From April 1, 1990 to July 1, 1998, this age group increased 34.1% by more than 1 million people as compared to the entire population which grew at a rate of 8.6%. At this rate of growth, in another 50 years, this age group would be about two-thirds as large as the current total US elderly aged 65+ of 35 million people. With a high probability of caregiving demand, this group would wipe out the current government programs design to pay formal caregivers.
Most elderly people in this country focus on providing the means to pay the high cost of medical services and drugs but tend to ignore the 6 fold times higher potential cost of long-term care. With the probability that government programs may not help them in the future, elderly Americans should shift their focus to providing the means to pay for the high cost of long-term care.
TRENDS IN CAREGIVING
In 1997, the national cost for home health care was $32 billion while the cost of nursing homes was $83 billion. This amounted to 10.5% of the total $1.1 trillion in health care costs for that year. This percent is projected to remain fairly stable through the year 2005.If we go back and add to the formal cost of care the estimated cost of $197 billion for informal care, we have a whopping 24% of the national health care budget devoted to caregiving.
Currently the government pays close to 40% of formal caregiving costs. If there were a future decline in the amount of available informal care accompanied by increase in demand for that care the government would be forced to absorb a great deal of those added costs. To put this in perspective bear in mind that Federal funding for Medicare is expected to run into deficit in the next few years and that state governments are already strapped in meeting public health care needs.
In 1997, Federal outlays for Medicare, Medicaid and other health programs were $367 billion. Adding in $140 billion in state and local spending, total government costs for health care in 1997 were $507 billion–about 46% of all health care cost, private and public. Payments for formal care absorbed $51.5 billion or 10% of government outlays already in that year. Had the government been forced to absorb the cost of informal care as well, it would have amounted to 35% of the budget and would have severely hampered the quality of other health services for 40 million Medicare recipients and millions more of Medicaid participants.
Could this happen? Is there currently a trend away from unpaid informal care towards paid formal care that could destroy the current public health care system?
Demographic trends over the past 50 years suggest that not only is the ratio of informal caregivers to those needing care getting smaller, but the availability of caregivers (living within the same community or state) in some regions of the country is also becoming a problem.
The national birthrate has been declining year over year while simultaneously the total number and percent of the population over 65 has been steadily increasing. From 1950 through 1999 the annual birthrate has declined from 24.1 per 1,000 to 14.5 per 1,000. At the same time the age adjusted death rate went from 5.9 per thousand in 1980 to 4.7 per thousand in 1998.
These statistics reveal that the younger population is growing more slowly while the older population is growing more rapidly. By the year 2050 the population over 65 is projected to grow from 12.8% of the total to 20.3%. Simple logic would show that the number of young caregivers is declining in proportion to a larger older generation that will inevitably need care. There is also a growing trend towards more households headed by single individuals. This will eventually reduce the number of healthy spouses available for caregiving as well.
As we learned from the section on cost of care, the need for caregiving increases with age. Compounding the challenges outlined above is the rapid growth of the very old age group which already accounts for over half of all nursing home residents and a large proportion of those needing community care. By the year 2050 this group will have grown from 4,333,000 people, today, representing 1.5% of the population to about 20,000,000 people, representing 4% of the population. Since this group has the greatest need for care, this trend will further deplete the numbers of available, future informal caregivers.
Finally, many potential caregivers have moved away and are not able to provide care for family or friends. This is particularly a problem for farmbelt states and rural communities where young people have left for better economic opportunities in urban areas. This trend shows no signs of reversing and the resulting lack of caregivers is putting great stress on affected communities and government programs.
If no solution is found for the loss of informal caregivers, much of the burden of providing care will shift to government-funded programs since no viable private sector alternative now exists. The added strain to an already underfunded senior health program could lead to a failure of the entire system.
THE PLIGHT OF INFORMAL CAREGIVERS
Caregiving can be very stressful and demanding. In the case of a healthy spouse or a child living with the disabled person at home, caregiving can be a 24 hour, 7 day a week commitment. But even for the caregiver not living in the home, looking after a loved-one or friend can consume all of the caregiver's free time.
Surveys and studies consistently show that depression is a major problem with full-time informal caregivers. This is typically brought on by stress and fatigue as well as social isolation from family and friends. If allowed to go on too long, the caregiver can sometimes break down and may end up needing long-term care as well.
A typical pattern may unfold as follows:
- 1 to 18 months--the caregiver is confident, has everything under control and is coping well. Other friends and family are lending support.
- 20 to 36 months--the caregiver is taking medication to sleep and control mood swings. Outside help dwindles away and except for trips to the store or doctor, the caregiver has severed most social contacts. The caregiver feels alone and helpless.
- 38 to 50 months--Besides needing tranquilizers or antidepressants, the caregiver's physical health is beginning to deteriorate. Lack of focus and sheer fatigue cloud judgment and the caregiver is often unable to make rational decisions or ask for help. It is often at this stage that family or friends intercede and find other solutions for care. This may include respite care, hiring home health aides or putting the disabled in a facility. Without intervention, the caregiver may become a candidate for long-term care as well.
Since most people go into informal caregiving without training or counseling they often aren't aware of the possible outcome described above. It is therefore extremely important to receive counseling and to formulate a plan of action prior to making a caregiving commitment. In 1965, Congress passed the Older Americans Act which provides guidance and funding to the States to give help to caregivers. All states offer programs at no cost or very low cost which might include: counseling, caregiver training, respite care, adult day care, meals, support groups and much, much more. IT IS VITAL FOR THE HEALTH AND LONGEVITY OF ALL CAREGIVERS TO MAKE USE OF THESE SERVICES.
We have seen that most caregiving in the US is provided in the community by unpaid, so-called informal caregivers. There is a growing trend towards fewer available caregivers trying to support a rapidly growing number of people needing care. This trend will require the use of more paid or formal caregivers and may greatly affect the ability of government to keep up with growing demand for paid care. Citizens should plan for ways to fund care for themselves. Finally, many don't know the effects that caregiving can have on mental and physical health. States offer help programs that include counseling, training and caregiver services.







